
What is the Link between Anti-Mullerian Hormone (AMH) and PCOS?
 PCOS (Polycystic Ovarian Syndrome) is also known as PCOD (Polycystic Ovarian Disorder). It’s considered to be a condition involving a hormonal imbalances. AMH (Anti-Mullerian Hormone) is one of the hormones associated with your ovaries. It is involved in menstruation, specifically in the formation of follicles in the ovary. Today, many experts regard AMH levels as one way of diagnosing PCOS and predicting infertility.
PCOS (Polycystic Ovarian Syndrome) is also known as PCOD (Polycystic Ovarian Disorder). It’s considered to be a condition involving a hormonal imbalances. AMH (Anti-Mullerian Hormone) is one of the hormones associated with your ovaries. It is involved in menstruation, specifically in the formation of follicles in the ovary. Today, many experts regard AMH levels as one way of diagnosing PCOS and predicting infertility.
+ Click here to learn about the all natural PCOS 5-Element Solution
+ Click here to read more articles about PCOS and Hormones
Symptoms
PCOS Hormones: The AMH (Anti-Mullerian Hormone)

Fertility clinicians are faced with the challenge of determining the degree of ovarian reserve to better tailor assisted reproductive technology treatment. Costly drug regimens, discomfort to patients, and the significant risk of complications associated with ovarian stimulation all justify the need for obtaining clinically relevant information before the commencement of treatment embarked on.
Many tests have been developed to screen for diminished ovarian reserve. Traditional methods used to predict prospective response to ovarian stimulation include mainly the measurement of baseline cycle day-3 serum concentrations of hormones such as FSH, estradiol, and inhibins. There are also ultra-sonographic tests for determining pretreatment ovarian volume and the number of early antral follicles. Recently, Anti-Mullerian Hormone (AMH), also referred to as Mullerian-inhibiting substance, has been proposed as a marker for predicting ovarian response to gonadotropin stimulation.10
Anti-Mullerian Hormone is a member of the transforming growth-factor beta super family. In women, it’s solely produced by the granulose cells of growing prenatal and small antral ovarian follicles. Serum AMH levels can be used as a marker of ovarian reserve, representing the quantity and quality of the ovarian follicle pool. Women with PCOS are known to have elevated baseline AMH levels when compared with age-matched ovulatory women according to a Taiwan study. Furthermore, one study in Italy concluded, “In our experience, AMH two or three times the normal amount (10 ± 2.28 ng/mL) is a good indication of PCOS and infertility.”
As a marker for ovarian reserve, MIS/AMH correlates positively with ovarian response to COH in norm-ovulatory women, but this has not been assessed in women with Polycystic Ovarian Syndrome (PCOS). Disturbed dominant follicle selection leading to an excess accumulation of prenatal and small antral follicles in women with PCOS presumably causes the elevated MIS/AMH levels.
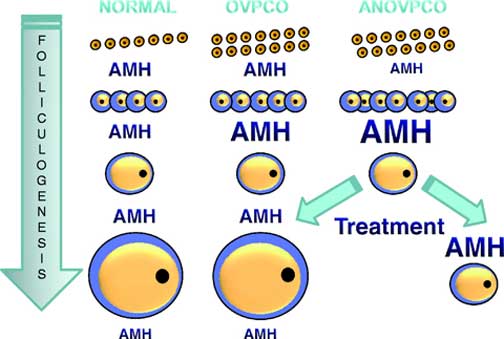
Although AMH has been shown to reflect antral follicle counts and to be elevated in PCOS, it is unclear how well measurements of AMH reflect ovarian morphological parameters in PCOS, specifically ovarian size and blood flow. Available literature does not reveal any study comparing assisted reproductive technology outcomes according to AMH levels between PCOS patients and non-PCOS patients. To gain further insight about AMH as a predictor of ovarian response, we investigated the relationship between the serum levels of Anti-Mullerian Hormone (AMH) and results of assisted reproductive technology in PCOS patients versus non-PCOS patients.11
Want to learn more about Insulin Resistance and its effects on your body?
Causes
Improve Insulin Resistance to battle AHM and PCOS Issues
 The present experimental study first evaluated the effect of Metformin administration on AMH concentrations assayed both on serum and follicular fluid in women affected by PCOS. Data confirms that AMH levels are significantly higher in PCOS patients than in healthy controls. A plausible hypothesis for this figure is that the increased AMH levels in PCOS are the result of the increased number of small ovarian follicles. In this regard, a direct and significant correlation between follicle number and serum AMH levels has been demonstrated by some authors.
The present experimental study first evaluated the effect of Metformin administration on AMH concentrations assayed both on serum and follicular fluid in women affected by PCOS. Data confirms that AMH levels are significantly higher in PCOS patients than in healthy controls. A plausible hypothesis for this figure is that the increased AMH levels in PCOS are the result of the increased number of small ovarian follicles. In this regard, a direct and significant correlation between follicle number and serum AMH levels has been demonstrated by some authors.
Interesting results were obtained by the evaluation of AMH levels in PCOS women who were treated with Metformin. In particular, we used as the study model PCOS patients who had a different response to Metformin administration in order to clarify the role of AMH in the ovarian response to the treatment. As already reported, our data seem to suggest that AMH might play a key role in the intra-ovarian mechanisms regulating the ovarian function.
In fact, significant changes in serum AMH levels in PCOS patients ovulating under Metformin, such as in those remaining anovulatory despite treatment were detected. The reason for the reduction in AMH concentrations after Metformin remains controversial. In a prospective study, Metformin acutely improved Insulin Resistance indexes and restored ovarian morphology, whereas no effect of the Metformin-induced improved insulin-sensitivity and AMH levels was observed. These data are strongly limited by the very small sample size and the short-term observation period. Moreover, Piltonen et al., in a prospective study, showed the AMH levels, the number of antral follicles, and ovarian volume were reduced after Metformin administration.
In addition, a positive correlation was found between serum AMH levels and both follicle count and androgen levels. These correlations were successively confirmed and a further relationship between AMH levels and Insulin Resistance indexes was demonstrated in untreated PCOS patients.9
On the other hand, in a recent prospective, randomized, double-blind, 26-week long-term study, AMH levels in untreated PCOS women seemed to be associated positively with testosterone, and negatively with DHEAS and C-peptide levels. Moreover, the same authors showed that six months of androgen suppression by either Metformin or low-dose dexamethasone treatment failed to influence circulating AMH level.
 The current study, confirming and extending previous data, suggests that Metformin acts on ovarian AMH levels with additive and direct mechanism of action. In fact, the effects of Metformin at ovarian site did not reflect those observed at systemic levels. Significant difference in intraovarian AMH levels was observed within PCOS patients who received Metformin on the basis of clinical response, even if women ovulating under Metformin maintained higher follicular AMH levels than healthy controls. Thus, it is possible to hypothesize that Metformin exerts a peripheral effect on the ovary by lowering AMH concentration that is detrimental for clinical response to the treatment.10
The current study, confirming and extending previous data, suggests that Metformin acts on ovarian AMH levels with additive and direct mechanism of action. In fact, the effects of Metformin at ovarian site did not reflect those observed at systemic levels. Significant difference in intraovarian AMH levels was observed within PCOS patients who received Metformin on the basis of clinical response, even if women ovulating under Metformin maintained higher follicular AMH levels than healthy controls. Thus, it is possible to hypothesize that Metformin exerts a peripheral effect on the ovary by lowering AMH concentration that is detrimental for clinical response to the treatment.10
Conversely, a slight effect on follicular AMH level was also observed in unresponsive PCOS patients; in fact, significant difference in AMH levels was observed between anovulatory PCOS women who had received Metformin and untreated anovulatory PCOS patients. A simple linear regression analysis was performed to establish the relationship between AMH in the follicular fluid and the systemic response to the treatment, which included Tand HOMA as indicators for improved hyperandrogenism and Insulin Resistance, respectively, and serum AMH.
As already shown, ovaries in the population with PCOS seemed to have a differential sensitivity to Metformin, and an improved biochemical response to Metformin by a “sensitive” ovary could be decisive for the clinical response mediated by AMH. In this regard, ovulatory patients with PCOS had significant correlations between the AMH levels in follicular fluid and the variation in plasma T and AMH levels and the variation in HOMA, respectively. On the contrary, patients with PCOS who were anovulatory under Metformin seemed to have a local “resistance” to the treatment, and no significant correlation between the variation in any systemic factors and follicular AMH levels was observed in these patients.11
Treatment Options
How to Address AMH Issues
 The study revealed that AMH is not a definite predictor for pregnancy and ART results in PCOS patients. Although it is proven that AMH measurement prior to gonadotropin stimulation could provide useful information to direct the application of mild patient-friendly stimulation protocols in order to avoid OHSS. Evaluation of patients who underwent Assisted Reproductive Technique (ART) is very important for both patients and physicians, because it is very expensive, time consuming, and stressful for patients. It’s important to predict who poor responders will be before starting the procedure. Nowadays many tests such as FSH, estradiol, antral follicle count (AFC), testosterone and free testosterone, for predicting ovarian reserve are suggested.11
The study revealed that AMH is not a definite predictor for pregnancy and ART results in PCOS patients. Although it is proven that AMH measurement prior to gonadotropin stimulation could provide useful information to direct the application of mild patient-friendly stimulation protocols in order to avoid OHSS. Evaluation of patients who underwent Assisted Reproductive Technique (ART) is very important for both patients and physicians, because it is very expensive, time consuming, and stressful for patients. It’s important to predict who poor responders will be before starting the procedure. Nowadays many tests such as FSH, estradiol, antral follicle count (AFC), testosterone and free testosterone, for predicting ovarian reserve are suggested.11
Thus, despite the different validity of these tests, there still remain patients who respond poorly to stimulation despite having normal tests of ovarian reserve. This supports the idea that ovarian reserve is not a simple static anatomic number and is not yet fully understood. Participants in our study had the same age, although despite their same mean BMI they seemed somewhat overweight. Basal characteristics (Including basal AMH) and cycle characteristics of the 89 patients were similar. In recent studies AMH has been proposed as a new method for predicting ovarian reserve.
According to Aflatoonian et al, small AFC and AMH are equally accurate predictors of high ovarian response to COH and allow us to identify the patients who are at increased risk of OHSS prior to the commencement of stimulation and help to determine the appropriate treatment protocols. AMH is the most significant predictor of embryo quality (AUC =0.728). It has the ability to predict poor and excessive response to stimulation with exogenous gonadotropins. This biomarker is superior to basal FSH and AFC, and has the potential to be incorporated into work-up protocols to predict a patient’s ovarian response.
On the other hand, serum level of AMH is a good predictor of the ovarian response to COH in norm-ovulatory women but not in PCOS. This study showed there was not a statistically significant difference between AMH level and pregnancy in PCOS in contrast to the control group. Wang et al, found that baseline MIS/AMH is not a good predictor of the ovarian response to COH in PCOS women. The arrest of follicular growth and the heterogeneity of FSH sensitivity among MIS / AMH-secreting follicles in PCOS render baseline measures of MIS/AMH a poor predictor of the gonadotropin response in PCOS.
However, there are few published studies confirming the relation between AMH and ovarian response in COH in this group of patients exclusively. In a recent study to relate follicular fluid AMH and FSH levels in patients with PCOS, it was suggested that the granulose cells from polycystic ovaries continue to produce elevated levels of AMH, possibly because of impaired access of FSH to follicles. Such an excess in follicular fluid AMH may have harmful consequences on oocyte quality and final maturation.
Polycystic ovaries have an abnormally rich pool of growing follicles and a disturbance in the selection and subsequent maturation of a dominant follicle. Increased serum AMH is due to increased production per granulose cell, suggesting an intrinsic granulose cell deregulation in PCOS. Not only is AMH expression increased, but it also might be protracted in polycystic ovary (PCO) follicles. The potential role of AMH on oocyte quality could be a future field of reproduction research.
There was not a significant relationship between AMH levels and pregnancy rate in our study. This raises the hypothesis of a negative link between AMH and final oocyte alteration. In the four studies, which evaluated the role of MIS/AMH in pregnancy prediction, two studies supported it and two studies did not. On the other hand, pregnancy rates after IVF are influenced by multiple (non-ovarian) factors including in vitro laboratory conditions, semen parameters, psychological stress, and technique of embryo transfer. Predicting response to gonadotropin treatment nevertheless remains an important aim in the evaluation of the couple struggling with infertility. Our study, despite its limitations like small sample size, has the benefit of comparing PCOS patients with a control (non-PCOS) group which recommends further well designed investigations in this regard.11
Natural Therapies
Adjusting Your Anti-Mullerian Hormone Levels Naturally
AMH (Anti-Mullerian Hormone) is one of the hormones associated with the ovaries. It is involved in menstruation, specifically in the formation of follicles in the ovary. Many experts regard AMH levels as an indicator of overall ovarian function, and testing for AMH levels is one way of diagnosing PCOS and predicting infertility.
 Metformin administration in ovulatory patients with PCOS exerts a differential action on the ovarian AMH levels on the basis of ovulatory response. Changes in AMH levels in antral follicular fluid during Metformin treatment could be involved in the local mechanisms mediating the ovulatory restoration. Further well-designed studies on a larger sample are needed before obtaining definitive conclusions.
Metformin administration in ovulatory patients with PCOS exerts a differential action on the ovarian AMH levels on the basis of ovulatory response. Changes in AMH levels in antral follicular fluid during Metformin treatment could be involved in the local mechanisms mediating the ovulatory restoration. Further well-designed studies on a larger sample are needed before obtaining definitive conclusions.
Until then there’s always a natural approach to address PCOS, which is Insulin Resistance. By eating a healthy diet – that means one that’s low in carbohydrates and sugars and high in fiber, fresh fruits and vegetables, you’ll have the ability to control your insulin levels. When that happens, you’ll better balance your hormones. By combining a healthy diet with a regular exercise and utilizing targeted nutritional supplements (specific blends of vitamins, minerals, and botanicals), you can reclaim your health.
Next Steps
- Take the PCOS Quiz! Get your score and assess your hormone health risks.
- Join our Facebook Sisterhood Group Pose your questions to this group of like-minded women. Get the answers to your questions and the support you need.
- Checkout the Hormone Reset. Guided Practices to eliminate anxiety, lose weight and boost energy.
We are committed to helping women reverse their symptoms of hormone imbalance – a major cause of excess weight gain, adult acne, unwanted facial hair, depression, anxiety, and heartbreaking female infertility.
©Insulite Health empowers women with hormone imbalance to transform their lives through a process of healing with the Natural Hormone Solution –a complete solution for helping women reverse the symptoms hormone imbalance..
