
How Can PCOS Affect Your Baby’s Weight?
 If you are pregnant and have PCOS you will be facing a time of incredible joy, as well as increased stress and worry about your growing baby. This is normal even for women without PCOS as well, but moms-to-be with Polycystic Ovarian Syndrome have more pregnancy problems than women who do not have this condition, so this stress might be intensified.6
If you are pregnant and have PCOS you will be facing a time of incredible joy, as well as increased stress and worry about your growing baby. This is normal even for women without PCOS as well, but moms-to-be with Polycystic Ovarian Syndrome have more pregnancy problems than women who do not have this condition, so this stress might be intensified.6
Polycystic ovarian syndrome (PCOS) is a disorder that is estimated to affect between 5-10 percent of women who are of childbearing age so you are not alone trying to manage this condition. PCOS seriously impacts a woman’s hormones, fertility, menstrual cycle, and appearance. One of the underlying influences of PCOS is a condition called Insulin Resistance, which can have a greater impact during pregnancy.6
What are the risks of a PCOS pregnancy?
Some of the health issues common for pregnant women with PCOS are:6
- Pregnancy-induced high blood pressure
- Miscarriage
- High blood sugar levels that can lead to gestational diabetes
- Premature delivery
- Pre-eclampsia
- Macrosomia (a newborn with an excessive birth weight)
These health issues are all serious, but addressing your PCOS symptoms as well as Insulin Resistance can help diminish some of the risks associated with a PCOS pregnancy. One factor to pay close attention to when pregnant is the prevalence of obesity in women with PCOS. Obesity increases the risk of developing gestational diabetes, which can cause excessive birth weight in the developing baby.8 High birth weight (macrosomia) is a common complication of a PCOS pregnancy and can compromise the health and future wellbeing of both mother and baby.
What is fetal macrosomia?
 Fetal macrosomia is used to describe a newborn who has a birth weight of more than 8 pounds, 13 ounces (4,000 grams) that occurs in about 9 percent of documented births worldwide. Large babies can cause a variety of complications for both the mother and baby both during and after the pregnancy. These complications increase when the newborn is more than 9 pounds, 15 ounces (4,500 grams).2
Fetal macrosomia is used to describe a newborn who has a birth weight of more than 8 pounds, 13 ounces (4,000 grams) that occurs in about 9 percent of documented births worldwide. Large babies can cause a variety of complications for both the mother and baby both during and after the pregnancy. These complications increase when the newborn is more than 9 pounds, 15 ounces (4,500 grams).2
The success of your pregnancy and the likelihood of having a normal weight baby can depend on how well you manage your PCOS, as well as the quality and frequency of the care you receive during your pregnancy. Consulting a doctor who is familiar with PCOS can be the key to creating an effective management plan, especially if you are overweight.6 It is important to be open to recommendations by your doctor concerning your diet, exercise levels, targeted nutritional supplements and medications or procedures that decrease the risks linked to PCOS pregnancies or fetal macrosomia.5
+ Click here to learn about the all natural PCOS 5-Element Solution
+ Click here to read more articles about PCOS and Pregnancy
Causes
High birth weight is definitely a possible complication of Polycystic Ovarian Syndrome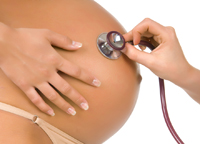
High birth weight is definitely a possible complication of Polycystic Ovarian Syndrome, especially if you are also obese.3 This does not mean PCOS causes fetal macrosomia but rather that obesity and conditions such as gestational diabetes associated with PCOS can cause larger babies. These issues can be managed with diet and exercise, as well as medication and managing your PCOS both before and during pregnancy, all of which can reduce the chances of pregnancy-related problems.
Possible causes of fetal macrosomia:
- Maternal obesity:? If you are obese, then having a baby diagnosed with fetal macrosomia is more likely.8
- Excessive weight gain during pregnancy:? The risk for a large baby increases if you gain a lot of weight during your pregnancy.4
- Maternal diabetes:? Women with PCOS have a greater chance of developing gestational diabetes and if this does occur or you have diabetes before your pregnancy, then there is a higher risk of fetal macrosomia, especially if you do not control your condition.4
- Overdue pregnancy:? Your baby might be larger If you are two weeks or more overdue.
- A history of fetal macrosomia:? If you were a large baby (over 8 pounds, 13 ounces at birth) or you have already had a baby with macrosomia, then you’re risk of having another one is higher.1
- Baby is a boy:? Boys tend to weigh more than girls, and most babies over the 9 pound, 15 ounce range are males.
- Previous pregnancies:? Babies seem to get larger with each successive pregnancy.
- Maternal age:? Older moms (over 35) tend to have larger babies.
- No risk factors: There is a very broad range of birth weights and some babies over 9pounds, 15 ounces have absolutely no risk factors, they are just big.1
A PCOS pregnancy can be characterized by pregnancy problems that can affect the baby and mother both before and after the birth. If your baby has been diagnosed with fetal macrosomia this can also present its own issues.
What are the maternal risks of fetal macrosomia?
Complications could include:1
- Issues during labor:? It will come as no surprise that large babies are harder to deliver than small ones. An oversized baby can get stuck in the birth canal causing injuries to the mother. If the situation does not resolve itself a C-section might be needed.
- C-Section: ?Any surgery carries risks such as infections, damage to organs, bleeding, and complications linked to general or local anesthesia.
- Issues after delivery:? After you give birth your uterine muscles contract and if they do not work properly because of a large baby serious bleeding can ensue.
- Uterine rupture:? Fetal macrosomia can cause scars from a previous C-section to tear which will force an emergency C-section to save both mother and child. This complication is rare but very serious.
- Genital Tears:? Babies diagnosed with fetal macrosomia can tear the perineum and vaginal walls during delivery.
What effect does fetal macrosomia have on the baby? 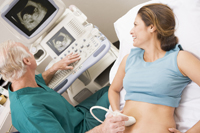
Several complications associated with fetal macrosomia can be passed on to your baby, so careful monitoring both during and after delivery is important. In most cases macrosomic babies do not suffer permanent damage or long-term effects.
Issues that might affect your baby stemming from fetal macrosomia are:
- High blood sugar level:? A baby with fetal macrosomia can be born with high blood sugar levels.7
- Metabolic syndrome:? Fetal macrosomia can increase the chance of your child developing metabolic syndrome, which is a group of interrelated conditions like high blood sugar, excess belly fat, and high blood pressure. This syndrome raises the risk of diabetes, stroke, and cardiovascular disease later in life.7
- Birth defects:? Babies that are large because their mother is obese during pregnancy have an elevated risk of being born with birth defects, like neural tube defects or heart conditions.2
- Childhood obesity:? Some studies have shown high birth weight can also mean greater risk of childhood obesity.7
- Injuries during delivery:? Birth trauma, including dislocated shoulders, is common for babies that have fetal macrosomia. Large birth weight babies can also sustain injuries to the facial nerves and the series of nerves connecting the spine to the extremities.1
- Death:? macrosomia is linked with neonatal morbidity, which is obviously the most serious concern for pregnant women.7
Symptoms
It’s challenging to definitively diagnose fetal macrosomia during pregnancy
One of the most interesting aspects of pregnancy is being able to track your baby’s 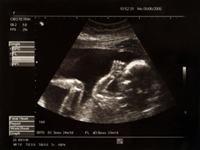 development through prenatal visits and seeing your baby on an ultrasound. Science and technology have come a long way, but it is still challenging to definitively diagnose fetal macrosomia during pregnancy. After all, the baby is inside and measurements through the belly of the mother are not always completely accurate.
development through prenatal visits and seeing your baby on an ultrasound. Science and technology have come a long way, but it is still challenging to definitively diagnose fetal macrosomia during pregnancy. After all, the baby is inside and measurements through the belly of the mother are not always completely accurate.
Some possible signs that might point to fetal macrosomia are:
- Larger than expected fundal height:? Prenatal visits are usually taken up by a series of measurements from the mother’s weight, to blood sugar and even the distance between the pubic bone and top of the uterus (fundal height). If this last measurement is larger than is normally found for the duration of your pregnancy it could indicate fetal macrosomia.1
- Polyhydramnios (excessive amniotic fluid):? Most people do not realize that part of the amniotic fluid that protects and surrounds the growing baby in pregnancy is actually made up of the urine output from the baby. The amount of urine in this fluid can reflect the size of the baby so in some cases excessive amniotic fluid can be a marker for fetal macrosomia.1
Natural Therapies
Lose weight naturally when you are overweight with PCOS
 The most important PCOS therapy to improve symptoms and reduce the risk of complications during your PCOS pregnancy is to lose weight if overweight.1 This almost immediately helps your body normalize its response to insulin and decrease the production of androgens. Even women with PCOS who are pregnant and have diabetes find that insulin therapy plus a healthy eating plan will cut the risk of macrosomia significantly.
The most important PCOS therapy to improve symptoms and reduce the risk of complications during your PCOS pregnancy is to lose weight if overweight.1 This almost immediately helps your body normalize its response to insulin and decrease the production of androgens. Even women with PCOS who are pregnant and have diabetes find that insulin therapy plus a healthy eating plan will cut the risk of macrosomia significantly.
Should I be more concerned about risks if I am obese?
Maternal obesity and excessive weight gain during pregnancy are considered to be two of the most influential factors when assessing the risk of macrosomia.8 For example, if you are obese before becoming pregnant you will double the risk of having a baby diagnosed with macrosomia.8 So it stands to reason that if you are overweight with PCOS you might want to consider dropping a few pounds before conceiving. It is also crucial to monitor your weight carefully urging your pregnancy to avoid gaining too much.2
If you have to pick the one thing you can do to support a healthy pregnancy, to reduce the symptoms of Polycystic Ovarian Syndrome, and to reduce the risk of a macrosomia baby, it would be eat a healthy diet.1 
A healthy diet can include:
- A reasonable amount of calories
- A pre-natal multivitamin
- Lean protein
- Fresh vegetables
- Fruit (but not in excess)
- Whole grains
- Healthy unsaturated fats
- Cut alcohol, sugar, caffeine, and saturated fats out of your diet if possible
Excessive weight gain during pregnancy can increase the risk of complications for you and your baby, especially if you are obese to begin with and have PCOS.6 You should monitor your weight carefully and only gain a healthy amount. Consult your doctor for a recommendation on how much weight would be healthy for you; every pregnancy is different.
.
How much weight should I gain during pregnancy?
The general guidelines concerning pregnancy and weight gain are:8
- Maternal weight normal before pregnancy: 25 to 35 pounds
- Single pregnancy and the mother obese: 11 to 20 pounds
- Multiple pregnancy and the mother obese: 25 to 42 pounds
Weight gain recommendations are just a suggestion, and you shouldn’t get completely caught up in standing on your bathroom scale. Simply be aware of the elevated risks of weight gain and obesity with respect to both macrosomia and Polycystic Ovarian Syndrome. Eat healthy foods in a reasonable quantity; engage in a regular daily exercise routine to minimize those complications, and take the time to enjoy the process of growing your baby.
Exercise
Exercise is an important component in controlling PCOS and help increase the body’s sensitivity to sugar.6 You can control your pregnancy weight gain by exercising, which is crucial for preventing macrosomia and alleviating common pregnancy discomforts such as back pain, constipation, cramps, and insomnia.8 The bottom line for a healthy pregnancy is to be physically active. If you are obese or have other medical issues, then consult your doctor about ways to be physically active without compromising your health or the health of your baby.
Treatment Options
There is no medical or drug course of treatment you can follow to prevent fetal macrosomia
There is no medical or drug course of treatment you can follow to prevent fetal macrosomia, but you can promote a healthy PCOS pregnancy by working closely with your doctor.6 If your doctor suspects fetal macrosomia there are recommended treatment options designed to help manage and even reduce the likelihood of the expected complications with a large baby.
Will I need specialized treatment during pregnancy if I am obese or have PCOS?
Many women with Polycystic Ovarian Syndrome are overweight and even obese, which can increase the chance of pregnancy problems and macrosomia.8 This means you will have to be monitored closely by your doctor and perhaps undergo treatment options designed to pinpoint the risk factors that will affect the health of you and your baby.
Depending on how well you are managing your PCOS and how your pregnancy is progressing your doctor might suggest:
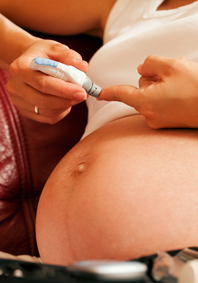 Manage diabetes:? If you had diabetes before pregnancy or you develop gestational diabetes, you must manage the condition to prevent macrosomia and the resulting complications from a large baby. Fetal macrosomia is less common when blood sugar is controlled. Drugs that normally treat diabetes, like Metformin, can be used to address Insulin Resistance, a common influencing factor of both PCOS and diabetes.5 Metformin is often recommended for pregnant women with PCOS who have a higher risk of babies with fetal macrosomia to improve their pregnancy problems and increase the likelihood of a positive outcome.8
Manage diabetes:? If you had diabetes before pregnancy or you develop gestational diabetes, you must manage the condition to prevent macrosomia and the resulting complications from a large baby. Fetal macrosomia is less common when blood sugar is controlled. Drugs that normally treat diabetes, like Metformin, can be used to address Insulin Resistance, a common influencing factor of both PCOS and diabetes.5 Metformin is often recommended for pregnant women with PCOS who have a higher risk of babies with fetal macrosomia to improve their pregnancy problems and increase the likelihood of a positive outcome.8- Early testing for gestational diabetes:? Women with PCOS have a greater risk of developing gestational diabetes and are often screened early using a test called the glucose challenge. Obesity in itself also increases your risk of gestational diabetes so the combination of the two conditions might mean the test is conducted as early as your first scheduled prenatal appointment. If the test is normal you will get a second test at the usual time between week 24 and week 28 of your pregnancy.6
- Fetal echocardiography:? Obesity in the mother sometimes raises the risk of birth defects affecting the heart, so a detailed image of the baby’s heart at 21 weeks can be used to rule out or confirm an issue.8
- Frequent prenatal visits:? The prevalence of PCOS pregnancy problems often prompts doctors to schedule more frequent prenatal visits, especially if the woman is also obese. This is a preventive measure and not cause for alarm.7
- Delayed fetal ultrasound:? Seeing your baby on an ultrasound during pregnancy is often a wonderful experience. However, PCOS-related obesity can make imaging difficult because ultrasound waves do not effectively penetrate abdominal fat. This procedure, usually performed between 18-20 weeks is sometimes put off until the pregnancy has progressed to get a better picture.8
Can I deliver my baby vaginally if Macrosomia is an issue?
Most pregnant women have very specific and detailed plans for the birth of their baby and nine months to think about it! It is often crushing when pregnancy problems like macrosomia derail those plans and a medical intervention like a C-section is recommended as the best option. Most doctors will err on the side of caution when there are concerns of macrosomia and suggest a C-section; however, this procedure is not always necessary. Many women with macrosomic babies do safely deliver vaginally although in some cases the labor is induced before the baby grows dangerously large. Induced labor is usually done when the mother wants to deliver naturally but it can’t always decrease the risks related to fetal macrosomia. A large baby delivered earlier always has the potential to cause damage.
A C-section might be the best option when you have diabetes or develop diabetes during your pregnancy which increases the risk of macrosomia.8 If you have PCOS your doctor will keep a close eye on all your tests and usually can accurately estimate the size of the developing baby. If the baby appears to be over 8 pounds, 13 ounces, a C-section is the safest method of delivery. If you do not have diabetes and your baby is estimated at 11 pounds, then your doctor will also counsel against a vaginal delivery. If a baby is too large one of the shoulders can actually wedge behind the mother’s pubic bone (shoulder dystocia) and this circumstance can be fatal for the baby. If you’ve delivered a baby with dystocia your risk increases of having the same issue. In this case a C-section is strongly recommended, especially if your risk factors of macrosomia are high. If this recommendation occurs before the 39th week of pregnancy, then a sample of amniotic fluid will be drawn to determine if your baby’s lungs are mature enough for a safe birth.
Next Steps
- Take the PCOS Quiz! Get your score and assess your hormone health risks.
- Join our Facebook Sisterhood Group Pose your questions to this group of like-minded women. Get the answers to your questions and the support you need.
- Checkout the Hormone Reset. Guided Practices to eliminate anxiety, lose weight and boost energy.
We are committed to helping women reverse their symptoms of hormone imbalance – a major cause of excess weight gain, adult acne, unwanted facial hair, depression, anxiety, and heartbreaking female infertility.
©Insulite Health empowers women with hormone imbalance to transform their lives through a process of healing with the Natural Hormone Solution –a complete solution for helping women reverse the symptoms hormone imbalance..
