Overview
What is PCOS?
 The Polycystic Ovary Syndrome (PCOS ) is a disease of the female sexual sphere which is characterized by the violation of the development of female sexual hormones, increase in the ovary sizes with the appearance of cysts, impairments of a menstrual cycle, infertility, and other symptoms.
The Polycystic Ovary Syndrome (PCOS ) is a disease of the female sexual sphere which is characterized by the violation of the development of female sexual hormones, increase in the ovary sizes with the appearance of cysts, impairments of a menstrual cycle, infertility, and other symptoms.
The reasons for the development of PCOS are unknown at present; however, it is supposed that a certain role in the development of this disease is played by hereditary factors, traumas, inflammatory diseases of genitals, etc. The PCOS diagnostics is based on the definition of characteristic symptoms, ovary ultrasound check-up, research of the level of hormones in blood, etc. The PCOS treatment depends on the age, weight, desires of a woman to become pregnant, and other factors; it also includes the normalization of body weight, hormonal or surgical treatment.
Causes
Why does PCOS develop?
The development of female sex hormones (progesterone and estrogen) in the female organism is under hypophyseal control: Follicle Stimulating Hormone (FSH) and Luteinizing Hormone (LH ) . During the menstrual cycle, the level of these hormones is not identical.
PCOS women have an increased level of LH and a decreased level of FSH, which leads to the disorders in the regulation of the menstrual cycle. The increased level of LH leads to the development of surplus of man’s sexual hormones (androgens) and estrogen in the female organism. The surplus of androgens promotes the development of diabetes, heart diseases, emergence of acne, etc. The raised level of estrogen and the lack of progesterone (which stimulates ovulation – the discharge of an egg from an ovary) leads to delayed ovulation, an excessive thickening of the inside layer of the uterus (endometrium) and to the development of amenorrhea (absence of menstruation), or uterine bleedings. In the majority of cases, PCOS is accompanied with obesity.
The exact causes of PCOS development are not known, however, there are the contributing factors the existence of which increases the risk of developing the above-mentioned illness:
- Hereditary factors (existence of PCOS at close female relatives);
- Chronic infectious diseases;
- Obesity;
- Abortions in the past;
- Pregnancy and childbirth with complications.
The Luteinizing Hormone (LH ) is a hypophyseal hormone, a regulator of the menstrual cycle and the formation of gonadal hormones at women, a stimulator of synthesis of testosterone at men.
“Luteinizing hormone (LH ) is produced by the pituitary gland in the brain. Control of LH production is a complex system involving hormones produced by the gonads (ovaries or testes), the pituitary, and the hypothalamus. Women’s menstrual cycles are divided into the follicular and luteal phases, characterized by a mid-cycle surge of follicle-stimulating hormone (FSH) and LH . The high level of LH (and FSH) at mid-cycle is supposed to trigger ovulation. LH also stimulates the ovaries to produce steroids, primarily estradiol. Estradiol and other steroids help the pituitary to regulate the production of LH . At the time of menopause, the ovaries stop functioning and LH levels rise”.
The glycoprotein gonadal hormone develops in the frontal lobe of hypophysis under the influence of luteinizing hormone of hypothalamus and sexual steroids (negative feedback). The level of LH is low up to full sexual maturity. During puberty, the cyclic secretion of gonadotropin, stimulating the development of genital glands and the secretion of sexual hormones, begins. LH secretion has a pulse character within days.
In women, LH stimulates the synthesis of an estrogen and regulates the secretion of progesterone and the formation of the yellow body. The concentration of LH changes during the menstrual cycle with the pre-ovulatory peak of concentration in the middle of the cycle (the concentration of LH considerably exceeds FSH level). The massed emission of LH during this period causes ovulation, formation of the yellow body, and transfer of biosynthesis of steroids on progesterone production.During the follicular and luteal phases, the estrogen makes negative return impact on LH development (except for the short period before LH peak in the middle of the cycle, when extradiol shows positive return action on LH secretion). During pregnancy, the concentration of LH becomes lower as a result of the elevated estrogen level. After menopause, the decrease of a braking return influence of steroids causes the increase of LH level.Follicle Stimulating Hormone (FSH) is a hypophysial hormone, a regulator of the development of ovary follicles in the female organism, and spermatogenesis at men. The absolute FSH concentrations are much lower than the concentration of LH . Reaching a critical level of FSH leads to ovulation. During the menopause, the reduction in concentration of extradiol causes an increase of FSH level.
FSH is one of the basic tests in diagnostics of pathology of the reproductive system, both at women and at men. The raised level of gonadotropin in combination with a low level of sexual steroids indicates the insufficiency of the function of sexual glands. The inadequate production of FSH reflects the dysfunction of the hypothalamo- hypophyseal axis.
Due to the pulsing nature of allocation of FSH and LH at conditions leading to the decrease in allocation of these hormones, it is recommended to take three consecutive samples of blood every 30 minutes. At the conditions connected with raised level of FSH (as, for example, at functional violations of sexual glands during the menopause), one test is necessary.
Symptoms
What are the signs of PCOS and abnormal LH levels?
At the gonadal causes of infertility, the increase in the concentration of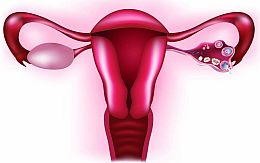 LH and FSH which is combined with a low concentration of sexual steroids is observed. Low concentration of gonadotropin and gonadal steroids are observed in the case of hypophysis hypo function. In some diagnostic situations, ratio of LH/FSH is important, which is in the norm at women to menarche, and is equal to 1, after a year menarche – from 1 to 1.5, in the period from two years after menarche up to a menopause – from 1.5 to 2.
LH and FSH which is combined with a low concentration of sexual steroids is observed. Low concentration of gonadotropin and gonadal steroids are observed in the case of hypophysis hypo function. In some diagnostic situations, ratio of LH/FSH is important, which is in the norm at women to menarche, and is equal to 1, after a year menarche – from 1 to 1.5, in the period from two years after menarche up to a menopause – from 1.5 to 2.
The indications to the analysis:
- Infertility;
- Premature delivery;
- Oligomenorrhea and amenorrhea;
- Premature sexual development and delay of sexual development;
- Growth delay;
- Sexual infantilism;
- Dysfunctional uterine bleedings;
- Syndrome of polycystic ovary;
- Endometriosis;
- Hirsuties;
- Control of hormonotherapy efficiency;
- Decrease of libido and potency;
- Definition of time of a probable ovulation;
- Researches connected with extra corporal fertilization;
Persistently high levels of LH testify to the situation when there is a violation of a normal negative feedback between gonads and hypothalamus, leading to the disinhibiting of hyperphysical production of LH and FSH. Such a situation is normal during the menopause, but it is a deviation from the norm during the reproductive period. It can testify to such conditions as:
- premature menopause;
- Turner’s syndrome;
- castration;
- Swyer syndrome;
- some forms of congenital hyperplasia of adrenal glands;
- ovary hypofunction.
Health Risks
What is the result of abnormal LH and FSH levels?
 The decrease in the sensitivity of peripheral tissues to insulin on the average by 50 % is revealed at PCOS at least 2-3 times more often than in the general population. This phenomenon has a universal character and is inherent in this pathology irrespective of the existence and degree of expressiveness of obesity – both at corpulent and thin patients of any age. The age and the size of surplus body weight define only the prevalence and intensity of insulin resistance at the level of liver, fatty, and muscular tissue.
The decrease in the sensitivity of peripheral tissues to insulin on the average by 50 % is revealed at PCOS at least 2-3 times more often than in the general population. This phenomenon has a universal character and is inherent in this pathology irrespective of the existence and degree of expressiveness of obesity – both at corpulent and thin patients of any age. The age and the size of surplus body weight define only the prevalence and intensity of insulin resistance at the level of liver, fatty, and muscular tissue.
“The test indicated that older girls, but not boys, of PCOS mothers had significantly higher concentrations of salivary insulin. Compared with the controls, the girls also had lower levels of urinary hormones. The key finding of the study is that insulin levels appear to be elevated in daughters of PCOS mothers, which becomes more pronounced as they pass through puberty. Since the androgen levels were comparatively normal throughout puberty, and insulin resistance was found only in girls who had undergone puberty, insulin is the primary problem, whereas male hormones are a secondary problem”.
The refraction of these cells to insulin involves a compensatory increase in the production of pancreatic endocrine hormone – hyperinsulinemia, which serves the reason for numerous adverse dismetabolic violations (breaking carbohydrate and lipid exchange). However, the sensitivity to insulin in androgen productive structures of ovaries and adrenal glands does not suffer, and in response to hyperinsulinism the development of man’s sexual hormones only increases, which aggravates the clinic of hyperandrogene.
Treatment Options
What can be done to reduce the effects of PCOS ?
The management of PCOS can include medication and there are many feasible choices with regard to drug treatment options so it is essential to examine the benefits, side effects and drug contradictions associated with each choice and discuss with your doctor what the best option is for you.
Some common treatment options for PCOS are:
Oral contraceptives: This can be the first and most common method used to regulate the menstrual cycle. These pills are available in a range of types that contain a combination of hormones, usually estrogen plus progesterone or just progesterone. You need to go over with your doctor precisely what you want to see when taking this drug before beginning a cycle.
This can be the first and most common method used to regulate the menstrual cycle. These pills are available in a range of types that contain a combination of hormones, usually estrogen plus progesterone or just progesterone. You need to go over with your doctor precisely what you want to see when taking this drug before beginning a cycle.
Metformin (Glucophage): Metformin is a drug which was produced for type-2 diabetics which increases insulin levels while controlling blood sugar. Since insulin resistance influences polycystic ovarian syndrome this drug is utilized to treat PCOS also with successful outcomes. Metformin appears to minimize PCOS symptoms and frequently helps normalize male hormone levels as well as and the menstrual cycle.
Male hormone blockers: These are generally used in combination with birth control pills to minimize unpleasant PCOS symptoms related to high levels of androgens. Birth control must be used in combination with these blockers due to the fact the blockers can cause birth defects in male fetuses. Some common choices of male hormone blockers are flutamide, finasteride and spironolactone.
PCOS Treatment from Insulite Health
Are you looking for PCOS natural treatment plans? Be sure to see what Insulite Health has to offer. As pioneers in natural, lifestyle?based remedies for PCOS we’ve helped countless women meet the challenge of Insulin Resistance. Be sure to explore our educational resources, blog, forum and support groups to see if our natural PCOS System might be your key to optimal health. Insulite Health is dedicated to helping you feel better and possibly reversing your PCOS so you feel more in control of your health. Get your free consultation with one of the Medical Staff on our Consulting and Advisory Team by contacting us today.
Bloom, Kathleen, ed. Prospective Issues in Infancy Research. Hillsdale, NJ: Lawrence Erlbaum Associates, 1981.
“Defining PCOS” (2012). The University of Chicago Medicine. Available at:http://www.uchospitals.edu/specialties/pcos/pcos.html#P66_4925
Eden, John. Polycystic Ovary Syndrome: A Woman’s Guide to Identifying and Managing PCOS. Crows Nest, N.S.W.: Allen & Unwin, 2005.
Eid, George M., Daniel R. Cottam, Laura M. Velcu, Samer G. Mattar, M.D.a, Mary T. Korytkowski, Gabriella Gosman, Pooneh Hindi, Philip R. Schauer. (2005). “Effective treatment of polycystic ovarian syndrome with Roux-en-Y gastric bypass”. Available at:http://my.clevelandclinic.org/documents/bariatric_surgery/PCOS .pdf
Froeschle, Janet G., Yvette Castillo, Mary G. Mayorga, and Terry Hargrave. “Counseling Techniques for Adolescent Females with Polycystic Ovary Syndrome.” Journal of Professional Counseling, Practice, Theory, & Research36.1 (2008): 17+.
“Gestational Diabetes on Rise”. The Daily Mercury (Mackay, Australia) 9 Feb. 2011: NA.
Han AR, Kim HO, Cha SW, Park CW, Kim JY, Yang KM, Song IO, Koong MK, Kang IS. (2011). “Adverse pregnancy outcomes with assisted reproductive technology in non-obese women with polycystic ovary syndrome: a case-control study”. Clin Exp Reprod Med. 2011 Jun; 38(2):103-8. Epub 2011 Jun 30.
Hart R, Norman R. (2006). “Polycystic ovarian syndrome-prognosis and outcomes”. 2006 Oct;20(5):751-78. Epub 2006 Jun 12. Available at: http://www.ncbi.nlm.nih.gov/pubmed/16766228
Heng, Boon Chin. “Should Patients Diagnosed with Polycystic Ovary Syndrome (PCOS ) Participate in Compensated Egg Sharing in Return for Subsidized Fertility Treatment?.” Human Reproduction and Genetic Ethics 15.1 (2009): 4+
“Hormonal Disorder Linked to Excessive Insulin.” Nutrition Health Review 1 Jan. 2009: 17.
Masharani, Umesh. (2008). “Diabetes Demystified”. New York: McGraw-Hill.Mitchell, Mary Kay. Nutrition across the Life Span. Philadelphia: W. B. Saunders, 1997.
“PCOS the Fertility Problem That Affects Me, Posh and One in Ten Women.” The Mail on Sunday (London, England) 20 June 2010: 28.
Pramik, Mary Jean (1996) “Hormonal Contraception and Diabetes: Select Carefully”. Drug Topics. Volume: 140. Issue: 13: 60+.
Next Steps
- Take the PCOS Quiz! Get your score and assess your hormone health risks.
- Join our Facebook Sisterhood Group Pose your questions to this group of like-minded women. Get the answers to your questions and the support you need.
- Checkout the Hormone Reset. Guided Practices to eliminate anxiety, lose weight and boost energy.
We are committed to helping women reverse their symptoms of hormone imbalance – a major cause of excess weight gain, adult acne, unwanted facial hair, depression, anxiety, and heartbreaking female infertility.
©Insulite Health empowers women with hormone imbalance to transform their lives through a process of healing with the Natural Hormone Solution –a complete solution for helping women reverse the symptoms hormone imbalance..
