
Why Do Women with PCOS Breastfeed Less?
Should You Be Concerned?

Can PCOS interfere with your ability to breastfeed? Researchers from Norways’s University of Science and Technology measured breastfeeding rates among new mothers. Their study revealed that an alarming 1 out of 7 women with PCOS were not breastfeeding, as compared to only 1 out of 50 in the non-PCOS group.1 Why do so many more women with PCOS find themselves not breastfeeding? If you are pregnant or trying to conceive, or if you are a new mother, you may be wondering whether PCOS could impair your ability to breastfeed your infant.
What exactly is the connection between PCOS and breastfeeding problems? Can you hope for a normal breastfeeding experience? Are breastfeeding problems inevitable with PCOS? What are the chances breastfeeding problems will impact you? And most importantly, what can you do to spare yourself and your child from the frustration of nursing difficulties?
The short answer is that breastfeeding involves many different hormones. An imbalance among these hormones can cause breastfeeding problems, such as low milk supply. Since women with PCOS often suffer from high levels of male sex hormones, they might be more prone to such problems. What sets off this hormonal imbalance in the first place? One answer is Insulin Resistance. Insulin Resistance is at the root of many PCOS symptoms and pregnancy problems, possibly including breastfeeding problems.
If you’re going through breastfeeding troubles right now, don’t despair! The good news is that PCOS need not rob you of a positive breastfeeding experience. In-depth information about breastfeeding and PCOS can be found in the tabs above, covering everything from causes to treatment options. Most PCOS women eventually resolve their issues and go on to have a close, nurturing breastfeeding relationship with their infant. Also, you can find solutions to many common breastfeeding problems from support groups like La Leche League International or from a Lactation Consultant.
+ Click here to learn about the all natural PCOS 5-Element Solution
+ Click here to read more articles about PCOS and Pregnancy
Causes
PCOS and Breastfeeding, what should you know?
 Medical experts agree – breastfeeding is the best feeding choice for infants.2 The World Health Organization and the American Academy of Pediatrics strongly recommend exclusive breastfeeding for the first six months of a child’s life. Breast milk supplemented with solid foods is recommended for the next 6-12 months and beyond.3, 4 On the strength of these recommendations, it is no wonder that many mothers hope to breastfeed their infants, and why they would be concerned about any obstacles or problems that might arise.
Medical experts agree – breastfeeding is the best feeding choice for infants.2 The World Health Organization and the American Academy of Pediatrics strongly recommend exclusive breastfeeding for the first six months of a child’s life. Breast milk supplemented with solid foods is recommended for the next 6-12 months and beyond.3, 4 On the strength of these recommendations, it is no wonder that many mothers hope to breastfeed their infants, and why they would be concerned about any obstacles or problems that might arise.
Hormonal Imbalances Can Cause Breastfeeding Difficulty
Breastfeeding involves a complex interplay of several hormones in the body. If you have PCOS, you already know that PCOS throws your hormones into a state of imbalance. In particular, elevated levels of male sex hormones, such as testosterone, often occur in PCOS (sometimes referred to as Functional Androgen Excess). This hormonal imbalance is responsible for many of the visible symptoms of PCOS, such as baldness and excess facial or body hair. Could excess male hormones also contribute to problems with breastfeeding? New research suggests a connection.
In 2008, a research study was conducted by Norway’s University of Science and Technology regarding the breastfeeding rate in new mothers suffering from PCOS. In this study, researchers measured the mothers’ levels of male hormones (androgens) during pregnancy and related those to their rate of breastfeeding. They hoped to discover whether having PCOS, with its unnatural elevation of male hormones, caused breastfeeding difficulty post-partum.
The study concluded that new mothers with PCOS have a more difficult time with breastfeeding, particularly in the early post-partum period of 1-3 months. The study revealed that 14 percent of the women with PCOS were not breastfeeding, compared to only 2 percent in the non-PCOS group.1 Fortunately, this disparity seemed to ease after the first three months.
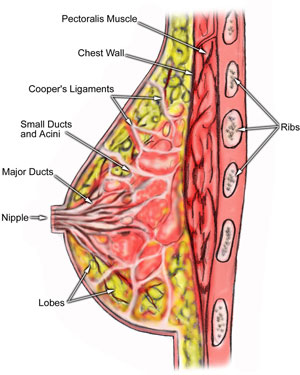
In a separate study conducted by lactation consultants in the United States, researchers reviewed specific cases of women with PCOS and breastfeeding difficulties. They noted an apparent connection between PCOS and low breast milk. Possible explanations are that PCOS interferes with proper development of the breast ducts (mammo-genesis), or with initiation of lactation in the alveoli (lactogenesis), or with secretion of breast milk through the nipple (galactopoiesis). Or PCOS could interfere with all three of these contributors to lactation and breastfeeding.5 The likely culprit in all cases is a PCOS-related hormonal imbalance.
Although it appears a correlation between PCOS and breastfeeding difficulty does exist, researchers are unsure exactly why. The Norwegian study hinted at an intriguing possibility: women with elevated levels of DHEA during pregnancy were more likely to encounter problems with breastfeeding later on. Could this be the missing piece of the puzzle?
DHEA is a precursor hormone which the body converts into the sex hormones estrogen and testosterone.6 Both of these hormones are closely involved in breastfeeding, and both are implicated in the hormonal imbalances of PCOS. Could the higher DHEA levels often seen in women with PCOS affect your supply of breast milk? Scientific research continues.
Symptoms
Is Your Milk Supply Really Low?
 A common reason cited by women who try breastfeeding, but give up, is low milk supply. But is your milk supply really low? Lactation Consultants report that women often believe their milk supply to be low, when in fact it is ample. Women often worry their milk supply is too low when their child’s nursing behavior changes, or they feel changes in their breasts. Neither of these is a true indicator of your breast milk supply! As long as your baby is gaining weight normally, there is little reason to worry about your milk supply.12
A common reason cited by women who try breastfeeding, but give up, is low milk supply. But is your milk supply really low? Lactation Consultants report that women often believe their milk supply to be low, when in fact it is ample. Women often worry their milk supply is too low when their child’s nursing behavior changes, or they feel changes in their breasts. Neither of these is a true indicator of your breast milk supply! As long as your baby is gaining weight normally, there is little reason to worry about your milk supply.12
What if your baby is exhibiting a failure to thrive by not weighing in the normal range? Low milk supply, a tricky and mysterious condition for healthcare providers, is a very likely culprit.5 Consult with your child’s pediatrician and/or a board-certified Lactation Consultant to assess the situation. Some women do legitimately struggle with inadequate levels of milk supply, and this symptom unfortunately can occur along with PCOS.
Complications
 Problems with breastfeeding is just one of many ways PCOS can complicate pregnancy and motherhood. PCOS (Polycystic Ovarian Syndrome) is the most common endocrine disorder in women of childbearing age, afflicting as many as 10 percent of women.7 In the United States alone, 7 million women suffer from this condition, which is especially heartbreaking since it erects so many obstacles to motherhood. If you have been dreaming all your life of becoming a mother, then be aware that this insidious hormonal imbalance can threaten your dreams of motherhood in several ways.
Problems with breastfeeding is just one of many ways PCOS can complicate pregnancy and motherhood. PCOS (Polycystic Ovarian Syndrome) is the most common endocrine disorder in women of childbearing age, afflicting as many as 10 percent of women.7 In the United States alone, 7 million women suffer from this condition, which is especially heartbreaking since it erects so many obstacles to motherhood. If you have been dreaming all your life of becoming a mother, then be aware that this insidious hormonal imbalance can threaten your dreams of motherhood in several ways.
PCOS is a leading cause of female infertility.8 If you have PCOS, then you confront the very real possibility of being unable to conceive.7 The hormonal imbalance of PCOS can lead to anovulation (when the ovaries do not release an egg) and menstrual irregularity. This causes infertility due to lack of ovulation.9
Even if you successfully conceive, you face an increased risk of miscarriage, premature delivery, and stillbirth.10 Women with PCOS also face higher rates of pregnancy-induced high blood pressure, gestational diabetes, and macrosomia (excessive birth weight).11 All of these conditions pose health risks for baby and mother. And as you’ve just learned, even after the baby is born, you face yet another challenge if you wish to breastfeed your newborn child.
Natural Therapies
Are you seeking natural solutions to your breastfeeding problems? Here are a few ideas to get you started.
Have you heard about the potential side effects from drugs and you seek a solution to your PCOS and breastfeeding problems without these risks? You’re in luck! There are several nutritional supplements that can produce positive results in managing the symptoms of PCOS. Botanicals and medications that increase the supply of breast milk are called galactagogues.
Common galactagogues with a reputation for safety include:
- Fenugreek (shown right)
- Blessed Thistle
- Alfalfa
- Brewer’s Yeast
- Fennel
- Anise
- Goat’s Rue
- Hops
- Milk Thistle
- Nettle Leaf
- Shatavari
- Flaxseed (shown right)
- Soapwort
- Marshmallow Root
- Red Raspberry Leaf
- Burdock
- Chaste Berry
Botanical supplements are often combined in order to maximize their effect. Two or three complementary botanical ingredients can accomplish more than using just one.13 A qualified naturopathic doctor, herbalist, or specially-trained nutritionist can help you select the right combination of botanical ingredients for PCOS.
Treatment Options
Don’t Give Up!
If you have PCOS and hope to breastfeed your child someday, or if you are currently experiencing trouble breastfeeding your baby, then don’t give up! There are many resources available, both online and locally, to help you resolve your issues and forge a successful, satisfying breastfeeding relationship with your newborn. Bear in mind that breastfeeding can be difficult for ANY new mom, not just women with PCOS. The issues you face may be more common than you think, and the solutions may be easier than you think.
Find Solutions to Your Breastfeeding Problems
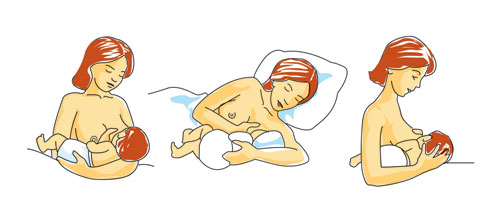
Sometimes all that is required to improve breastfeeding success is nursing more frequently, re-positioning the baby for a better latch, adding or taking away pumping sessions, etc. Sometimes the baby needs to grow and mature just a tiny bit more so his mouth can more effectively extract the milk. The mother might also need to improve her nutritional status and hydration.2 A certified Lactation Consultant or experienced La Leche League leader can assess your situation and recommend the best course of action.
An excellent resource for addressing breastfeeding difficulties is La Leche League International (www.llli.org). This organization of volunteers has chapters all over the world with women ready and willing to help out new mothers who are having problems establishing or maintaining breastfeeding. Also, your midwife or obstetrician can refer you to a certified Lactation Consultant for professional assistance. Another excellent online resource to remedy breastfeeding problems is www.kellymom.com.
Having a baby introduces numerous changes into the family and can create emotional upheaval and physical stress, even when the child is welcomed by the family! So don’t feel like a failure if you are having trouble with this seemingly most basic of bodily functions – it takes practice, patience, and sometimes a little coaching. Also remember that nursing is not an ‘all or nothing’ affair. When necessary, you can supplement your breast milk with formula or donated breast milk. There is nothing wrong with that! Any nursing you do, any breast milk you provide, goes a long way toward establishing the maternal-neonatal bond and nurturing the physical and emotional health of both you AND your child.
Most breastfeeding problems can afflict both women with PCOS and women without the condition. The reason women with PCOS suffer additional breastfeeding challenges is the subject of ongoing research. The excess male sex hormone levels (androgens) that accompany PCOS are believed to be at the root not only of breastfeeding difficulties, but many other problematic symptoms associated with PCOS.
Next Steps
- Take the PCOS Quiz! Get your score and assess your hormone health risks.
- Join our Facebook Sisterhood Group Pose your questions to this group of like-minded women. Get the answers to your questions and the support you need.
- Checkout the Hormone Reset. Guided Practices to eliminate anxiety, lose weight and boost energy.
We are committed to helping women reverse their symptoms of hormone imbalance – a major cause of excess weight gain, adult acne, unwanted facial hair, depression, anxiety, and heartbreaking female infertility.
©Insulite Health empowers women with hormone imbalance to transform their lives through a process of healing with the Natural Hormone Solution –a complete solution for helping women reverse the symptoms hormone imbalance..
