
Your BMI Could Be Hurting You (And … PCOS Might Be Why)
Most people have heard of the term, “Body Mass Index” or BMI for short. Unfortunately, for a lot of us, that term often conjures up painful images of physical education class lectures and embarrassing physical testing in school gyms. And typically, once we passed our physical education classes, we almost immediately forgot about that sometimes-sensitive topic, Body Mass Index. But did you know that BMI is actually a valuable measurement tool that can actually play a positive role in your Polycystic Ovarian Syndrome (PCOS)? Understanding Body Mass Index is an important aspect of maintaining a thorough comprehension of one’s health; for both men and women. But for women with PCOS (Polycystic Ovary Syndrome), it’s crucial for you to fully understand how your Body Mass Index or BMI relates to your hormonal disorder. While the root cause of PCOS symptoms is Insulin Resistance, the good news is you can have greater control over your health, and weight, by making some simple and healthy lifestyle choices.
“Body Mass Index” or BMI for short. Unfortunately, for a lot of us, that term often conjures up painful images of physical education class lectures and embarrassing physical testing in school gyms. And typically, once we passed our physical education classes, we almost immediately forgot about that sometimes-sensitive topic, Body Mass Index. But did you know that BMI is actually a valuable measurement tool that can actually play a positive role in your Polycystic Ovarian Syndrome (PCOS)? Understanding Body Mass Index is an important aspect of maintaining a thorough comprehension of one’s health; for both men and women. But for women with PCOS (Polycystic Ovary Syndrome), it’s crucial for you to fully understand how your Body Mass Index or BMI relates to your hormonal disorder. While the root cause of PCOS symptoms is Insulin Resistance, the good news is you can have greater control over your health, and weight, by making some simple and healthy lifestyle choices.
Symptoms
What Is PCOS?
PCOS (Polycystic Ovarian Syndrome) is an endocrine disorder that causes an imbalance of female to male hormones in women. The endocrine system is a system of glands which release hormones into the bloodstream to regulate the body’s daily functions.1 Each woman naturally produces androgens, which are “male” hormones; but in many women with PCOS (Polycystic Ovarian Syndrome), these androgens (or male hormones) are produced at a higher rate. The body normally does a good job of balancing itself out; however, hormones flow throughout your entire body and are responsible for a variety of important bodily functions. So, in women with PCOS, this excess male hormone called androgen especially affects the reproductive system.
The ovaries release female reproductive hormones. When there is an excess of androgen, creating a hormonal imbalance, the natural female reproductive functions are interrupted. Without the proper level of female hormones, ovulation is not triggered. Without the release of an egg (a process called ovulation), a woman cannot get pregnant. Additionally, menstrual cycles (the monthly shedding of an unfertilized egg and the uterine wall) are thrown off by the reproductive system’s inability to stick to the natural cycle because of the hormonal imbalance created by the excessive amount of androgen.
The female reproductive system plays a large role in the identity of a woman especially in regard to her dreams of becoming a mother. For many women with PCOS (Polycystic Ovarian Syndrome), these dreams feel as though they have been permanently destroyed. Although it’s possible for a woman with PCOS to become pregnant, the devastating symptoms of Polycystic Ovarian Syndrome can make it very difficult to conceive.
system plays a large role in the identity of a woman especially in regard to her dreams of becoming a mother. For many women with PCOS (Polycystic Ovarian Syndrome), these dreams feel as though they have been permanently destroyed. Although it’s possible for a woman with PCOS to become pregnant, the devastating symptoms of Polycystic Ovarian Syndrome can make it very difficult to conceive.
Health Risks
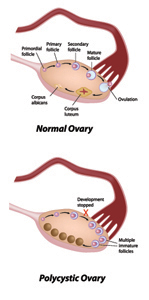
To make this highly emotional and painful situation even worse, there are no agreed-upon and definitive diagnostic criteria for Polycystic Ovarian Syndrome. Frustratingly, the health risks of PCOS manifest differently in different women. Most experts consider that a woman must have evidence of both lack of ovulation manifested by irregular periods AND signs of excess male hormones to be diagnosed with PCOS. Some experts also require the presence of polycystic ovaries (small cysts resembling a string of pearls) to confirm a diagnosis of PCOS.
Medical professionals must make their diagnosis of PCOS based upon a combination of blood tests, family history and a list of diverse and confusing symptoms, which occur in different combinations from one woman to another. These risks can include (but are not limited to) the following:
- Infertility
- Weight gain or obesity
- Missing (amenorrhea), heavy/excessive (menorrhagia) or irregular (oligomenorrhea) menstrual periods
- Skin conditions: including acne, skin tags, oily complexion, dandruff and the development of dark brown or even black, rough patches of skin (acanthosis nigricans)
- Anxiety
- Depression
- Sleep apnea
- High cholesterol
- Hair loss (male pattern baldness)
- Excess growth of hair (hirsutism); on the face, chest, stomach, thumbs or toes
- Ovarian cysts
- Pelvic pain
PCOS (Polycystic Ovarian Syndrome), often attributed to Insulin Resistance, is also a condition that can lead to more serious, and sometimes fatal, illnesses, especially if left untreated. These illnesses include coronary or cardiovascular heart disease, breast cancer, diabetes and endometrial cancer.
Causes
What Are Insulin Resistance and Body Mass Index?
Polycystic Ovarian Syndrome is a condition that stems from Insulin Resistance (IR). IR causes a negative disruption in the natural process of converting glucose to energy. The results? High blood sugar levels and weight gain. Body Mass Index, or BMI, is a measurement of body fat. Every person is built differently, and determining whether a woman is healthy based solely on their weight reading, is tricky. Many women can weigh a “healthy” amount (in terms of the number of pounds or kilos). But, at the same time, they can have an unhealthy, large percentage of body fat. Your BMI is very important because it provides a better gauge of whether you need to lose (or gain) body fat. And for women with PCOS (Polycystic Ovarian Syndrome), gaining weight easily is a typical and distressing PCOS symptom.
Simply put, Body Mass Index (BMI) is a ratio between your height and weight. A woman who is taller will weigh more than one who is shorter; so using a proportion rather than a scale will determine a more accurate reading of one’s overall health. At first glance, determining your BMI may seem a bit complex; but it’s really just a matter of plugging your personal numbers into the formula below.
To find your Body Mass Index,  follow this formula:
follow this formula:
- Take your weight (lbs) and divide it by height (total inches).
- Take the result of that calculation and divide it by height again.
- Then, multiply that number by 703.
- Round to the second decimal place to get your BMI.
For example, let’s say Nadine is 5’5” (65” total) and weights 126 lbs. Her weight by height would be 1.938461538. When that number is divided by 65 again, the figure comes out to 0.029822485. When multiplied by 703, she gets her BMI of 20.96 or 21.
So, What Does Your BMI Mean?
A Body Mass Index is a number that indicates whether someone is:
- Underweight (a number less than 18.5)
- Normal weight (a number between 18.5 – 24.9)
- Overweight (a number between 25.0 – 29.9)
- Obese (a number more than 30)
In our scenario above, Nadine would be considered normal weight since her number was 21. For most people, the Body Mass Index is simply a gauge that accurately tells them whether or not they are overweight. However, for women who suffer from PCOS (Polycystic Ovarian Syndrome), the Body Mass Index can also act as a lifesaving compass, guiding them toward a healthier lifestyle. Keep in mind though, not all women who suffer from PCOS are overweight. Nadine could be experiencing PCOS just the same as another woman who registered at 31 and is considered obese.
For the mothers, daughters, sisters and wives that are struggling with PCOS symptoms on a daily basis (currently estimated at five to seven million in the United States alone3), understanding and tracking their BMI is akin to finding themselves on a map. If their BMI has gone up (they are farther away from their ultimate destination), their diet needs to be tweaked or their exercise routine needs to be enhanced. On the other hand, if their BMI has gone down (they are closer to their ultimate destination), their current lifestyle is helping them to lose weight and possibly helping them combat their Polycystic Ovarian Syndrome.
What is the Relationship Between BMI and PCOS?
Does PCOS cause weight gain, or does weight gain cause PCOS? While it is unknown whether PCOS causes weight gain, or whether the causality is the other way around, it is known that reducing BMI into the normal range is associated with a lessening of other PCOS symptoms, such as infertility, acne or hirsutism. Obesity influences not only the severity of PCOS symptoms, but also increases risks of serious health problems.
weight gain cause PCOS? While it is unknown whether PCOS causes weight gain, or whether the causality is the other way around, it is known that reducing BMI into the normal range is associated with a lessening of other PCOS symptoms, such as infertility, acne or hirsutism. Obesity influences not only the severity of PCOS symptoms, but also increases risks of serious health problems.
Obese women with hyperandrogenism (high levels of male hormones) often have a characteristic distribution of body fat. Known as android obesity, central body obesity, or apple obesity, this type of obesity causes weight to be concentrated in the midsection. This fat distribution pattern is considered dangerous as it is associated with hyperlipidemia (high fat in the blood), type 2 diabetes, heart disease, and abnormal metabolism of sex steroids, which results in increased androgen production and suppression of sex hormone-binding globulin SHBG.
Elevated BMI by itself can have adverse effects on becoming pregnancy and pregnancy outcome, which means that obese women have a lower chance of becoming pregnant and, once pregnant (either via fertility treatment or spontaneously), have a greater chance of miscarriage. But what’s really going on in your body to explain the link between weight gain and the risks of infertility from PCOS?
Natural Therapies
How Can Women with PCOS Lower Their Body Mass Index?
Two of the most common and frustrating consequences for women who struggle with the disorder of Polycystic Ovarian Syndrome include increasing weight gain and the seemingly inability to lose that weight. Not only do these symptoms affect your health, but they also create a significant and devastating impact on your confidence and self-esteem.
Our culture today often places a great deal of importance on a thin body image. Yet sadly, even for a fit woman, these image expectations may be unrealistic, unattainable and most importantly, unhealthy. Particularly when combined with the unhealthy trend towards losing weight at any cost.
What’s vital for women with PCOS to understand is that current fad diets will do nothing to help them to lose the weight and regain their health. If you’re battling Insulin Resistance, the solution to lowering your BMI (and restoring your health) lies not in crash diets, but in a well-rounded and healthier lifestyle.
- If you have Polycystic
 Ovarian Syndrome you should begin incorporating a diet high in fiber and complex carbohydrates (such as vegetables) and low in sugars, fats and simple carbohydrates. By choosing lots of vegetables and some whole grains and fruits (in proper serving sizes), you can begin to minimize the interference of Insulin Resistance (the underlying cause of PCOS) and restore your body to converting glucose to energy in a more natural manner. Incorporating lots of vegetables along with some whole grains and fruits will also provide a substantial source of fiber to help fight high cholesterol (another symptom of Polycystic Ovarian Syndrome which can lead to heart disease).
Ovarian Syndrome you should begin incorporating a diet high in fiber and complex carbohydrates (such as vegetables) and low in sugars, fats and simple carbohydrates. By choosing lots of vegetables and some whole grains and fruits (in proper serving sizes), you can begin to minimize the interference of Insulin Resistance (the underlying cause of PCOS) and restore your body to converting glucose to energy in a more natural manner. Incorporating lots of vegetables along with some whole grains and fruits will also provide a substantial source of fiber to help fight high cholesterol (another symptom of Polycystic Ovarian Syndrome which can lead to heart disease). - Consistent exercise or movement is also important in effectively overcoming the difficult challenges of Polycystic Ovarian Syndrome, lowering your Body Mass Index and losing weight. However, because PCOS presents so many different health issues, if you’re dealing with this hormonal disorder you must incorporate exercise at your own rate and always in conjunction with the advice of your doctor. For some women, this may mean going to the gym five days a week; for other women, it may mean taking a walk around the block every morning. By working with your personal physician, you can both determine the best activity, intensity and duration for your body and in view of your medical history. As is often true, more is not always better. Your doctor can help you make the best decision for your health and safety.
- Incorporating nutraceuticals is a
 potent and natural way to improve your overall health, particularly in the presence of PCOS. As specialized blends of herbs, vitamins and minerals, nutraceuticals are designed to target specific ailments and boost overall well-being in a natural way with fewer side effects than traditional drugs. Choosing the right nutraceuticals may seem daunting at first, but with a basic understanding of how these supplements work, you can enhance the success you achieve with restoring your health.
potent and natural way to improve your overall health, particularly in the presence of PCOS. As specialized blends of herbs, vitamins and minerals, nutraceuticals are designed to target specific ailments and boost overall well-being in a natural way with fewer side effects than traditional drugs. Choosing the right nutraceuticals may seem daunting at first, but with a basic understanding of how these supplements work, you can enhance the success you achieve with restoring your health.
Using BMI to Control PCOS
While there is no cure PCOS can be managed. As you begin to address the debilitating PCOS symptoms naturally, you’ll find that your Body Mass Index is just one of the most effective tools at your disposal. Without a doubt, your BMI will act as an invaluable compass guiding you in your journey back to optimal health.
Resources
“Understanding Ovulation,” American Pregnancy Association, March 2011, http://americanpregnancy.org/gettingpregnant/understandingovulation.html, 16 September 2011.
“Polycystic Ovary Syndrome: Symptoms & Treatments for PCOS,” The Hormone Foundation, 16 September 2011.
Yildiz BO, et al. (2008). “Impact of Obesity on the Risk for Polycystic Ovary Syndrome”. J Clin Endocrinol Metab. 93 (1): 162–168.
Next Steps
- Take the PCOS Quiz! Get your score and assess your hormone health risks.
- Join our Facebook Sisterhood Group Pose your questions to this group of like-minded women. Get the answers to your questions and the support you need.
- Checkout the Hormone Reset. Guided Practices to eliminate anxiety, lose weight and boost energy.
We are committed to helping women reverse their symptoms of hormone imbalance – a major cause of excess weight gain, adult acne, unwanted facial hair, depression, anxiety, and heartbreaking female infertility.
©Insulite Health empowers women with hormone imbalance to transform their lives through a process of healing with the Natural Hormone Solution –a complete solution for helping women reverse the symptoms hormone imbalance..
